Illustrated by Erin Rommel & Sabrina Bezerra
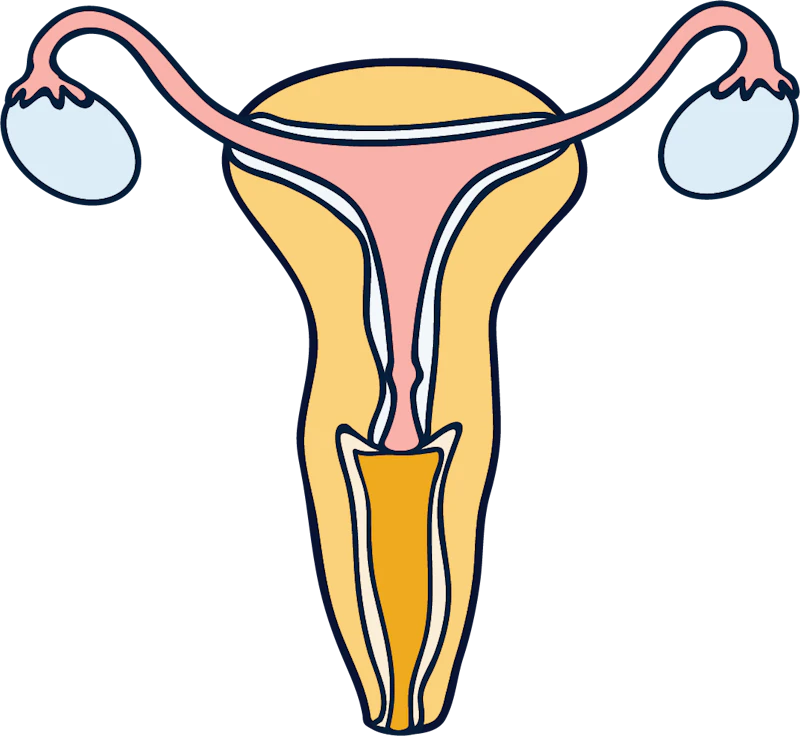
Pelvic inflammatory disease, or PID, is an infection that affects the upper part of the reproductive system—your uterus, ovaries and fallopian tubes.
Alongside causing severe pain and heavy periods, pelvic inflammatory disease can cause serious long term problems, including infertility.
It’s a condition that you may never heard of, which is surprising when it mostly affects women who’re sexually active and between the ages of 15 and 24. Despite the age bracket you won’t find it discussed in sex education in school, meaning that many who get it only find out about it for the first time when they’re diagnosed.
How do I know? Because I was one of those people.
After severe pain, my legs in stirrups, swab after swab and several gloved hands teamed with a whole lot of lube I was given the verdict: pelvic inflammatory disease.
Symptoms
The problem with PID is that many of its symptoms are similar to other conditions—severe cramping can be mistaken as period pain, unusual vaginal discharge might be an STI, etc.
Some people might not experience any symptoms at all, where others like myself might feel everything from extreme pain around the pelvis to bleeding between periods.
Even if you do get mild symptoms you’ll probably experience one of the following:
- Pain in the lower abdomen—it can be on both sides or sometimes you might feel it just on the right.
- Discomfort during penetrative sex, namely pain that can be felt deep inside your pelvis.
- Bleeding between periods and after sex.
- Heavy and painful periods.
- An unusual discharge from your vagina that can be yellow or green and has a foul odour.
- Painful urination.
If you’re really unlucky (I’ll raise my hand here) you might get really unwell with:
- A high temperature.
- Nausea and being sick.
- Severe abdominal pain.
For me it felt like someone had lit a match right behind my belly button and no matter how many painkillers I took or hot water bottles I filled, nothing eased it.
My period had decided to join the party (because clearly I didn’t have enough to contend with) and I couldn’t use tampons because it just hurt deep inside way too much. It wasn't an STI, so what the hell was going on?
Causes
Pelvic inflammatory disease is caused by an infection, and yes, sometimes an STI can be responsible.
In the majority of cases PID appears when an infection in your cervix (the opening to the womb) spreads into the womb itself as well as the fallopian tubes and ovaries.
In the UK, about 1 in 4 cases of pelvic inflammatory disease will be caused by an untreated STI —namely chlamydia or gonorrhoea. If left untreated the bacteria can travel up the reproductive system and kick-start a case of PID.
According to the NHS, 1 in 10 people with untreated chlamydia may develop pelvic inflammatory disease within a year, so if there was ever a reason to get regular STI check-ups let this be it.
But what about people like me?
Unfortunately in many cases the cause of pelvic inflammatory disease is completely unknown, sometimes normal bacteria that lives in the vagina can just decide to go walkabout and get past the cervix.
There are things that can make you more susceptible to PID however. You’re at more risk of pelvic inflammatory disease if you have unprotected sex and are under the age of 25. Some evidence also suggest you’re also more at risk of pelvic inflammatory disease in the first 4 to 6 weeks after having an IUD fitted, but the risk is very low.
Diagnosis
Diagnosing PID is no easy feat as there’s no simple test for it. Instead, it’s diagnosed through a combination of vaginal examinations and an overall assessment of your symptoms.
The first thing your doctor will do is feel inside your vagina to see how tender you are. I accidentally kicked my gynaecologist in the side of the head so that should give you an idea of how tender we’re talking. Because pelvic inflammatory disease is so tricky to diagnose, there’s a chance your doctor will ask someone else to give a second opinion—or in my case a third.
You’ll also be asked to chat through your sexual history and take an STI test. A positive test makes it easier to diagnose PID. Swabs are taken from your cervix and the inside of the vagina to look for evidence of any bacterial infection.
Other testing can include:
- A pregnancy test.
- A urine test.
- A blood test.
- An ultrasound.
- In rare cases a laparoscopy might be used. A thin camera is inserted and tissue samples might be taken but this is usually to rule out other conditions such as appendicitis.

Treatment
Treating pelvic inflammatory disease is fortunately very easy.
As PID is usually caused by a nasty combination of different bacteria, treatment involves taking a combination of different antibiotics. This’ll usually start before your swabs are back from the lab and you’ll take them for 14 days. My course was kickstarted with a single antibiotic injection in my bum cheek.
It’s really important that you finish the whole course of antibiotics. If the infection doesn’t properly clear that’s where complications can come in. Not to ruin the fun, but sex is also off the table for the duration of your treatment.
To ease abdominal pain while undergoing treatment, painkillers such as ibuprofen and paracetamol can be prescribed or bought over the counter.
Usually after three days of treatment a doctor will hold a follow-up appointment to check that treatment is working.
Your sexual partners may also be asked to undergo antibiotic treatment, even if an STI test comes back negative.
It’s important that you take treatment seriously: 1 in 10 people who get pelvic inflammatory disease will become infertile as a result and this is mainly due to delaying treatment.
TL;DR
- Pelvic inflammatory disease, or PID, is an infection that affects the upper part of the reproductive system.
- Some people might not experience any symptoms at all, where others might experience everything from extreme pain around the pelvis to bleeding between periods.
- PID is caused by irregular bacteria infecting the womb, and 1 in 4 cases will be caused by an STI
- Treatment includes taking a combination of antibiotics. If untreated, pelvic inflammatory disease can cause infertility and chronic pelvic pain.







