Table of contents
1. Stress and sex hormones
2. Stress and the thyroid
3. Stress and insulin
4. Stress and melatonin
5. Supporting stress resilience
Illustrated by Sabrina Bezerra, Erin Rommel & Ralitza Nikolova
Stress is a normal – and necessary – part of everyday life. But if you’re experiencing chronic stress and high cortisol symptoms you may notice a knock-on effect on your other hormones. Knowing how to lower stress hormones is an essential tool for feeling more balanced in your cycle, and yourself.
Stress gets a pretty bad rap. It’s commonly associated with negative symptoms like poor sleep, anxiety, digestive issues and irritability. And those certainly can be signs of chronic or intense stress. But some stress is essential: an uptick in our stress hormone cortisol is what gets us out of bed in the morning. Appropriate levels of stress also motivate us, fuel our productivity and help us to respond quickly if we’re in danger.
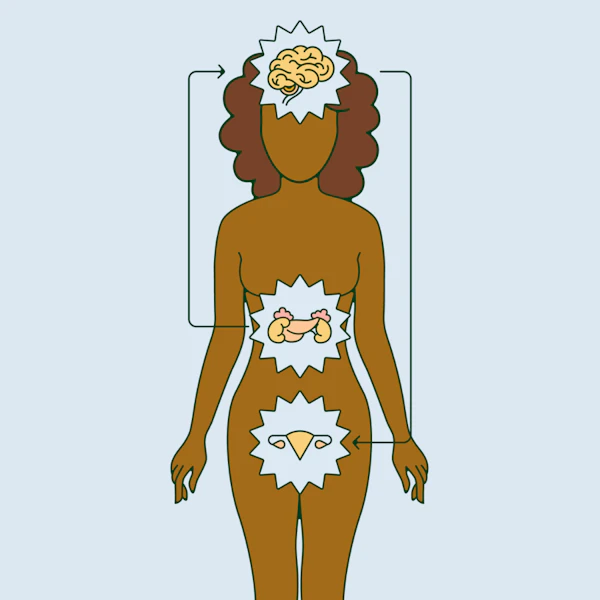
The body’s response to stressors is the same whether they’re physical (a car racing towards us as we cross the road) or psychological (an argument or a short-term work crisis). In these moments, the brain registers the stressor and sends messages via the sympathetic nervous system to the adrenal glands, which pump out adrenaline and cortisol. These stress hormones then activate certain processes in the body, putting it into ‘fight or flight’ mode. The communication process that controls these actions is the hypothalamic-pituitary-adrenal (HPA) axis.

In the ‘fight or flight’ state, you feel more alert and energised; your muscles are tense, your heart-rate is faster and you take quicker breaths. In a normal stress response, once the threat has passed, your parasympathetic nervous system kicks in to calm you down. The stress response’s ability to adapt in this way is healthy and desirable.
However, when stress becomes chronic – when we are living with constant or repetitive stressors – the adaptation of this response is compromised and our other hormones are affected. The cycles these hormones help to regulate can then get out of whack.
Stress and sex hormones
Just as the brain sends messages to the adrenal glands to release stress hormones, it also communicates with the ovaries about which hormones to release at different points in the menstrual cycle.
The brain’s perception of stress affects the communication of these messages, altering the release of the sex hormones oestrogen and progesterone. This can show up as shorter cycles, PMS, anxiety and even missed or absent periods.
Outside of cycle changes, chronic psycho-social stress has been shown to result in reduced libido and female reproductive and sexual function. Dys-regulated sex hormones can also impact mood and the immune system.

Stress and the thyroid
The thyroid is a butterfly-shaped gland in the neck, which produces hormones that control the body’s metabolism.
The thyroid is highly sensitive to stress. Elevated stress hormones can interfere with thyroid hormone production and the conversion of thyroid hormones into their active form. But compromised thyroid hormones can also make you more susceptible to feeling stress, creating a vicious cycle.
Hypothyroidism (low thyroid function) is the most common thyroid dysfunction, and is a slowing down of the body’s metabolic rate. Some of the classic symptoms are fatigue, low mood, anxiety, weight gain or difficulty losing weight, constipation, intolerance to cold and dry skin. Women may also experience menstrual cycle changes and more intense PMS.
“
Chronic stress and its effect on blood sugar increases the risk of insulin resistance.
Stress and insulin
Insulin is released by the pancreas and regulates blood sugar. It’s the hormone that transports glucose from our blood into our cells where it can be used for energy.
The relationship between cortisol and insulin is an important one as it’s part of the primal ‘fight or flight’ stress response.
Cortisol inhibits insulin release and encourages the release of glucose stores from the liver. This increases the amount of glucose in the bloodstream, where it can be readily available for energy when we need to fight or flee.
Chronic stress and its effect on blood sugar increases therisk of insulin resistance. Because blood sugar regulation is fundamental to a number of hormonal interactions this impacts various systems in the body, including sex hormone balance (insulin resistance is commonly seen inPCOS), immune system function, inflammation and cardiovascular health.
Stress and melatonin
Cortisol is a key player in the body’s natural circadian rhythm. When functioning normally, cortisol peaks in the morning to wake us up, then steadily decreases throughout the day, allowing melatonin - our sleep hormone - to rise in the evening. Because cortisol and melatonin have opposing effects, the rise of each is dependent on the fall of the other.
When cortisol doesn’t follow this natural pattern, melatonin is suppressed at night. This is one of the reasons why problems sleeping are such a common symptom of stress.

Supporting stress resilience
A resilient and adaptive stress response will support hormonal balance. So here’s how to lower stress hormones when they become intensely activated.
· Reduce caffeine. While it may make you feel more alert, caffeine activates the body’s stress response at a time when it’s already dialled up. If you still need a hit, replace coffee and black tea with green tea – it’s got less caffeine and also contains l-theanine which elevates GABA and serotonin; your calming and feel-good neurotransmitters.
· Breathe deeply. This helps to activate the parasympathetic nervous system and regulate the stress response. Try to extend your exhale so it is longer than each inhalation. By tuning in to when you feel your breath becoming more shallow or quick, you can identify when you need to regulate.
· Keep your blood sugar steady by minimising refined carbohydrates and sugary foods and including a serving of protein such as nuts, seeds, beans, legumes, eggs, fish, meat or poultry with every meal.
· Prioritise sleep. Stress is very physically and emotionally demanding, so giving your body time to rest and repair is especially important. Focus on keeping the time you go to bed and wake up each day consistent. Also build in a calming bedtime routine and minimise screen time in the evenings (ideally go screen-free for at least an hour before bed).