Illustrated by Erin Rommel
Corona, Covid, whatever you want to call it, there’s a new C-word on the block, meaning cancer (the OG C-word) has taken a back seat during the pandemic.
But while the world might be on pause, cancer certainly isn’t – and the coronavirus pandemic is affecting the cervical screening programme in more than one way.
Cancer referrals are down by up to 80% in some areas since the start of COVID-19. Are fewer people getting cancer? No, of course they’re not. But fewer people are going to their GP with potential symptoms, which will ultimately result in more people being diagnosed with cancer at a later stage. According to the gynaecological cancer charity The Eve Appeal, nearly 1 in 3 women who didn’t go for a cervical screening were put off by COVID.
There are over 3,000 cases of cervical cancer every year in the UK, which in the ‘cancer world’ is a relatively low number, but that’s because the screening programme saves over 4,000 lives each year.
Cervical screening, or smear tests as they are commonly known, is an effective way of detecting abnormal cervical cells that could develop into cancer if left untreated. But then COVID-19 happened, cervical screening appointments were (and still are) cancelled or delayed and to be quite honest, it’s really unclear what’s going on.
I run Ask Eve, the free information service for The Eve Appeal. Our mission is to see fewer people diagnosed with a gynae cancer and more people survive. We want to stop these cancers before they start and believe that prevention is better than cure.
Cervical cancer is a mostly preventable disease, and the only one of the gynae cancers that has a free NHS screening programme.
Bearing in mind that The Eve Appeal is a gynae cancer charity, not a cervical cancer charity, well over half of the people I speak to via Ask Eve are asking about their cervical screening or colposcopy (the procedure you’re referred for if you receive an abnormal screening result) appointment. It’s a huge concern for some people, and anxiety levels have understandably gone through the roof. Here’s what’s happening:
Why was cervical screening put on hold?
Seeing patients for non-urgent appointments stopped at the start of the pandemic. GPs moved these appointments telephone/video calls when possible, although how you do a smear test via Zoom is beyond me.
As cervical screening does not test for cancer, is not classed as ‘urgent’. Cervical screening tests for high-risk HPV, and if HPV is detected, the sample will then be tested for abnormal cells. It is completely separate to the cancer referrals I previously, well, referred to.
Cancer referrals are for GPs who suspect a cancer, or want to rule out a cancer, and screening is a routine procedure for the ‘healthy’ population.
Have cervical screening stopped in the UK?
In 2020 the cervical screening programme were paused in Scotland, Wales and Northern Ireland, but have now resumed in Scotland. It was never given a red light in England, but I would say that since the start of lockdown screening has been operating on a VERY heavy amber level, with almost all surgeries postponing appointments. COVID has affected the cervical screening programme and colposcopy referral process, so many are still experiencing delays.
Has cervical screening started again now restrictions are easing?
NHS England called for cervical screening appointment and reminder letters to be sent out as normal from 6th June 2020, but you just might need to wait a little longer for the appointment than pre-Covid times, as there is going to be a backlog of tests to catch up with.
Towards the end of last May, NHS England instructed GP surgeries to resume cervical screening appointments, but only if they are able to. Vague and annoying, I know.
It really does depend on which GP surgery you are registered to, and this explanation can be incredibly frustrating for some people. If your GP surgery isn’t currently booking in appointments, keep phoning and checking for an update.
Will people who are at higher risk be given priority?
Yes. People who are at a higher risk of cervical cancer will be given a priority appointment for their cervical screening, i.e. they will be seen sooner than someone who for example hasn’t had an abnormal result in the past and is currently due for their routine 3-yearly test.
You are considered ‘higher risk’ if you have HIV, are taking immunosuppressant medication, have persistent high-risk HPV, are due a follow-up appointment after receiving treatment for abnormal cells or a previously abnormal screening result.
Are cervical screening appointments different during COVID?
Other than the nurse or doctor wearing a mask and gloves, the actual screening procedure itself is no different. But, when you get to the surgery, you will need to phone the reception and let them know you have arrived, and wait either outside in a socially distanced queue, or in your car.
The receptionist will check that you don’t have any potential coronavirus symptoms, and if you do, you won’t be able to have your screening. You will either be phoned or collected when your nurse or doctor is ready for you, met at the surgery doors and escorted directly to your appointment room. There won’t be any time spent waiting in the… you guessed it, waiting room.
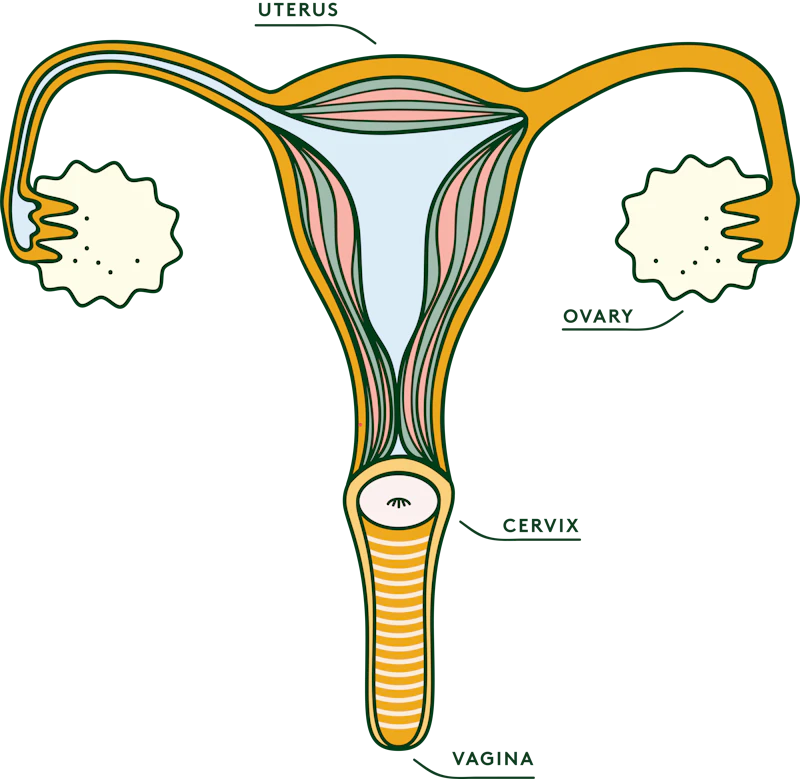
What happens if I receive an abnormal result after my cervical screening?
It’s a bit different to the years BC (before Covid). About 1 in 20 cervical screening results will come back as ‘abnormal’. If you receive an abnormal cervical screening result, you would normally be referred for a colposcopy, to investigate the abnormalities and decide if treatment is needed.
Abnormal cells are also called CIN (Cervical Intraepithelial Neoplasia), and are graded as CIN1, CIN2 and CIN3. The number depends on how far into the surface of the cervix these abnormal cells have developed. The higher the grade, the deeper the abnormal cells can be found. CIN1 often returns to normal and doesn’t need treatment, CIN2 sometimes requires treatment to remove the abnormal cells, and CIN3 is always removed as these cells are closer to becoming an early cervical cancer if left untreated.
In the years BC, you would be invited for a colposcopy whether you had CIN1, 2 or 3. In the current climate (I had to stop myself from typing ‘unprecedented times’), only people with CIN3 are being seen for a colposcopy, as these cases are more urgent than CIN1 and 2.
Staff availability, patient safety, risks versus benefits and hospital resources are all taken into consideration. This temporary ‘rule’ that means some people with abnormalities get a hospital colposcopy appointment and some don’t, is causing high levels of stress amongst both groups. People I speak to who had either their colposcopy booked in before lockdown and then subsequently cancelled as their results weren’t ‘bad’ enough, or who can’t get a colposcopy appointment in the first place because their recent results show mild rather than severe cell changes, are incredibly worried that their cell changes will progress to a cancer in the time they have to wait.
The British Society for Colposcopy and Cervical Pathology (BSCCP) has issued guidelines stating that it is safe for women in this position to have their colposcopy appointment deferred by up to three months.
This is because it typically takes years, and I’m talking years for HPV to develop from the virus into cervical cancer, so waiting a few extra months carries an extremely low risk of those cells progressing to the next stage. With that in mind, it won’t surprise you that I’m speaking to people who have got their colposcopy appointment coming up, and are equally as frightened because their cell changes are severe enough to warrant a priority appointment and much more urgent investigation.
Abnormal cells don’t mean cancer, CIN3 isn’t the same as early cancer, and that over 90% of people who have abnormal cells removed will never require additional treatment.
Although it’s safe for appointments to be delayed, it takes years for HPV to develop into anything serious, I know how upsetting this might be, and how scary it is to ‘just wait’. I almost got through this article without mentioning my story, but it’s the penultimate paragraph now, so screw it.
I had cervical cancer a few years ago, hence my borderline obsessive interest in cervical screening, HPV and all the jazz that goes along with this disease. The effects the cancelled appointments are having on people’s mental health are far greater than the physical impact these delays will cause.
If you experience any potential cervical cancer symptoms – bleeding in between periods, after sex, after the menopause being the main signs, and pelvic pain/pain during sex and a bloody/unpleasant smelling discharge being less common symptoms – you need to speak to your GP, who will be able to refer you to your local hospital’s gynae department.
If you have potential cervical cancer symptoms, you do not need a cervical screening test, you need a gynaecology referral and these are still happening, with or without a pandemic.
If you’re unsure about your screening appointment, phone your GP. If you have concerns about your colposcopy appointment, phone your hospital’s colposcopy team. Or, if you want to speak to someone before either of those phone calls, come and talk to me. Email nurse@eveappeal.org.uk and Tracie (the amazing gynae nurse I run Ask Eve with) or I will reply quickly and we can go through any questions you might have.
Just because it’s safe to wait, it doesn’t mean the waiting isn’t scary!