Table of contents
1. What is a chemical pregnancy?
2. What are the symptoms of chemical pregnancy?
3. What causes a chemical pregnancy?
4. What to do after a chemical pregnancy?
Illustrated by Ralitza Nikolova
It remains somewhat of a taboo subject matter, yet miscarriage — the unexpected and spontaneous loss of a foetus within the first 24 weeks of pregnancy — is estimated to impact as many as one in five pregnancies. But did you know there's more than one type of miscarriage, and many of us don't know about the most common kind?
What is a chemical pregnancy?
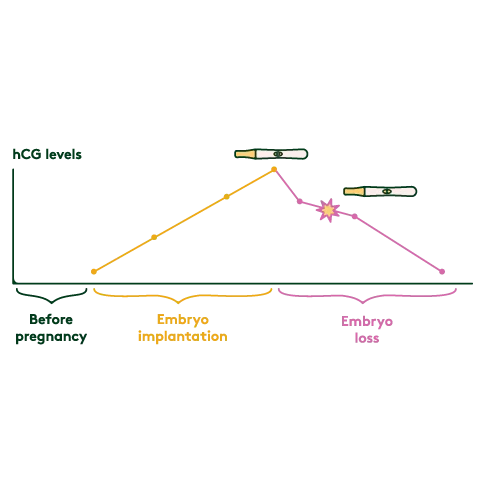
While it might sound like something out of a science lab, a chemical pregnancy is a name given to a miscarriage that occurs early on. “They usually happen within the first five weeks of pregnancy, just after the embryo forms and then implants, but then stops developing,” explains Dr. Ellie Rayner, obstetrician, and gynaecologist.
Later in the first trimester, miscarriages are typically detected and confirmed via an ultrasound scan. But routine scans aren’t typically offered until around 11 weeks into the pregnancy — long after the five-week time frame for a chemical pregnancy has passed.
As such, “a chemical pregnancy is diagnosed when a pregnancy has been confirmed by either a blood test or a urine pregnancy test,” reveals Professor Arri Coomarasamy, consultant gynaecologist and spokesperson for the Royal College of Obstetricians and Gynaecologists.
However, because this type of miscarriage occurs so early, some people don’t even realize they might be pregnant in time to take a test. Instead, they “mistake the bleeding for a normal or later period,” says Dr. Rayner. In fact, it’s estimated that up to 75% of pregnancies end before a positive pregnancy test result is even obtained, meaning the actual number of chemical pregnancies is likely significantly higher.
What are the symptoms of chemical pregnancy?
With no scan to confirm a pregnancy or miscarriage, it can be trickier to recognize a chemical pregnancy — especially as “symptoms can vary from person to person,” Dr. Rayner shares.
One of the most common signs to note is “vaginal bleeding, like a period”, she continues. “This can vary, and some women may find it is lighter or heavier than their normal period. You may also notice some small blood clots.”
If you’ve had a positive pregnancy test and then start to experience bleeding, you “may need blood tests to find out what’s happening,” explains Professor Coomarasamy (you can speak to your GP about getting these). “If these tests show that pregnancy hormones are decreasing or absent, a woman will be diagnosed as having an early pregnancy loss.”
Aside from bleeding, cramping in the lower abdomen is another primary indicator — but, again, this can easily be mistaken for period pains.
Either way, whether you’ve had a positive test or not, “if you are experiencing any bleeding that is unusual for you, particularly during pregnancy, we would encourage you to see a doctor,” states Professor Coomarasamy.

What causes a chemical pregnancy?
Following a miscarriage, it’s easy to blame yourself and question if you could have done anything to prevent it. But Professor Coomarasamy explains it’s important to recognize that “often the reasons for miscarriage are beyond [your] control.” So what’s going on, then?
As is the case with miscarriages throughout the first 12 weeks, “the most common cause [of chemical pregnancy] is a chromosomal problem, which is usually random and ‘one-off’ and can’t be prevented,” Dr. Rayner reveals.
Research indicates that at least 50% of miscarriages in the first-trimester result from chromosome abnormalities, such as improper formation or missing genetic information.
Other factors thought to potentially increase your risk of experiencing a chemical pregnancy include having underlying health concerns, such as polycystic ovary syndrome (PCOS), diabetes and thyroid issues, or being over the age of 35.
Frustratingly, “it is not always possible to know why a miscarriage happens,” states Professor Coomarasamy. “This can mean that miscarriage is difficult to come to terms with, as many are left with unanswered questions.”
What to do after a chemical pregnancy?
Miscarriage at any stage of pregnancy — planned or otherwise — can be a highly distressing and emotional experience. “Everyone may experience different feelings, and people may need support to help them come to terms with it,” Professor Coomarasamy says.
All feelings are valid, and it’s crucial to understand that you’re not alone. “If anyone is struggling with grief after a miscarriage, support is available from the charity Tommy’s, which has an online community and helpline,” he continues.
What about the physical aspect? If you’re actively trying to get pregnant and experience a chemical pregnancy, you might wonder how long you have to wait until you can safely restart your conception journey.
Aside from making sure you feel emotionally ready to try again, “most doctors will recommend waiting until after your next period before trying to conceive again,” explains Dr Rayner. “This will ensure you have completely recovered and will make a future pregnancy easier to date and manage.”