Table of contents
1. What is menopause (and perimenopause)?
2. What is the relationship between menopause and the vaginal microbiome?
3. Can I reduce my menopause symptoms?
4. Is there a link between probiotics and menopause symptoms?
Illustrated by Erin Rommel, Sabrina Bezerra & Ralitza Nikolova.
“I am just exhausted all the time,” says 57-year-old Karen Green, author and entrepreneur. “[I have] headaches, cannot tolerate alcohol and got achy joints into the bargain. Oh, and bizarrely cannot remember how to spell!”
Karen is talking, of course, about the menopause: her fatigue and achy joints are emblematic of the bodily process that everyone with a uterus will go through at some point during their life.
Of course, not everyone experiences menopause symptoms; but for those who do, those symptoms can have an enormously debilitating impact on both physical and mental wellbeing.
That said, it’s possible those symptoms could be reduced with certain strategies. We won’t get ahead of ourselves, though; in order to establish helpful strategies, it’s first worth recapping on just what exactly happens in the body during menopause.
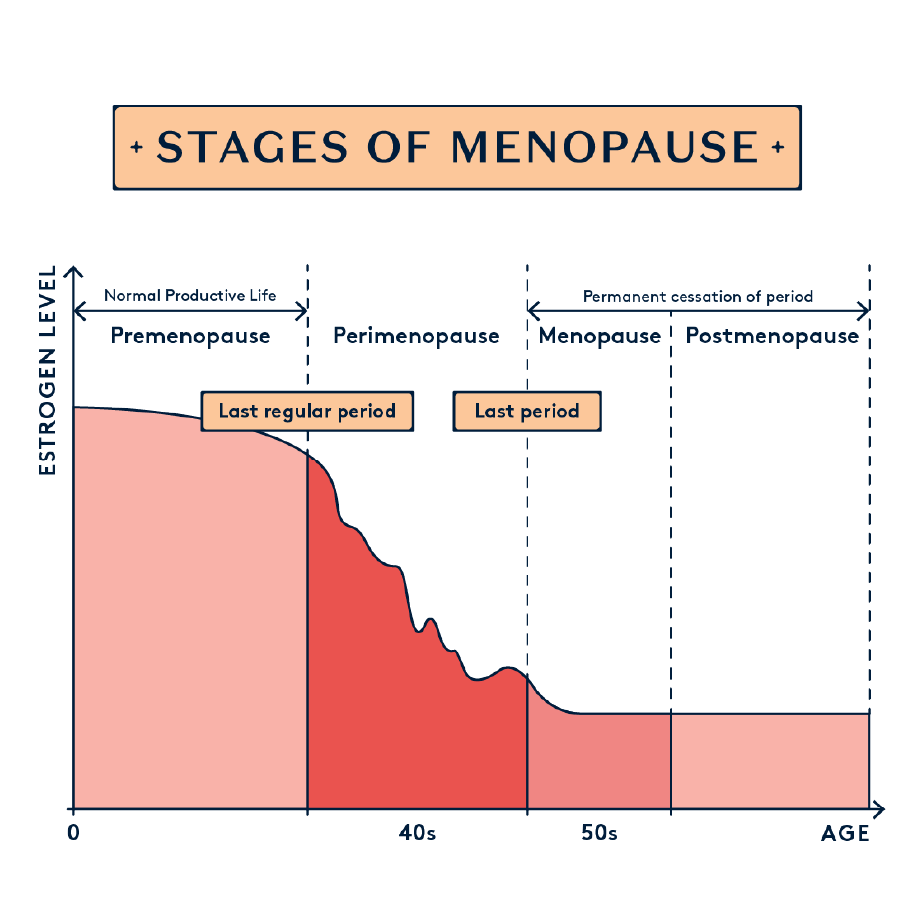
What is menopause (and perimenopause)?
Barbra Hanna, DO, FACOG, NCMP is Founder & CEO at MyMenopauseRX. “Menopause is the time when one’s ovaries stop producing hormones and periods stop,” she says. “Menopause can be surgical or natural.” The average age in the UK for someone to reach menopause is 51; but early menopause (occuring in someone’s 20s, 30s or 40s) can occur, too – this is something that affects around 5% of women.
Perimenopause, meanwhile, is the time leading up to menopause. “It can begin in a woman’s late 30s [or] early 40s and continue for years,” Hanna explains. “You can experience perimenopause even with regular periods.” And Hanna also points out that “perimenopause is like PMS on steroids for many women!”
47-year-old Consumer Champion Jane Hawkes suspected she could be perimenopausal last year. “I was teary, irritable, at times irrational in my thoughts, had problems with brain fog, concentration and memory and was suffering extreme anxiety, night sweats and mood swings,” she tells me. “As I have Multiple Sclerosis it was hard to know whether I was feeling the way I did because of it, or because I was perimenopausal.” The perimenopause was posited by a nurse following a cervical screening, though; and when it was confirmed by a doctor, Jane was hugely relieved to have an answer.
Symptoms of menopause include, among others:
And, of course, there are the myriad ways in which menopause can affect the vagina, such as vulvovaginal atrophy (VVA): a ‘genitourinary symptom of menopause’ which affects over half of postmenopausal women. “My vaginal wall is more fragile than it once [was]”, adds Karen.
Why does menopause have such a big impact on the vagina? Well, it has a lot to do with the oestrogen and the vaginal microbiome…
What is the relationship between menopause and the vaginal microbiome?
Essentially, oestrogen is needed to keep a low vaginal pH and a healthy vaginal microbiome; but during menopause, oestrogen levels fall significantly.
“Vaginal health is directly related to oestrogen,” Hanna explains. “The vagina, vulva and bladder all have oestrogen receptors. When oestrogen levels [decrease during] menopause, the vagina’s natural acidic environment becomes disrupted, leaving postmenopausal women to have reduced levels of intravaginal lactobacilli.”
And lactobacilli is what a healthy vaginal microbiome is all about. We’ve previously rooted for lactobacilli to become a household name, and we’re standing by that now. “Lactobacilli help keep our vaginal microflora balanced,” says Hanna. “If this balance is off, women are at greater risk of vaginal infections like bacterial vaginosis (BV) and vulvovaginal candidiasis (VVC)” – the latter of which is commonly known as a yeast infection.
Together with the increased risk of infections, other vaginal symptoms of menopause include:
- Thinning of the vulva;
- Painful sex;
- Increased urgency and frequency of urination.
One might well ask, then…

Can I reduce my menopause symptoms?
“Each menopause journey is unique and there is no one size fits all treatment,” Hanna says. She explains that menopause symptoms can be reduced by “lifestyle interventions [such as] some over the counter supplements [and] cooling devices you wear or sleep on.”
Let’s go into more detail. Lifestyle interventions for reducing menopause symptoms could include:
- Cutting down on caffeine and alcohol, which “can help you avoid hot flushes and enhance the quality of your sleep,” according to The Association of UK Dieticians, which also suggested the following dietary tip…
- Eating “at least four to five portions of unsalted nuts, seeds and legumes a week”;
- Using a handheld or electric fan, which can help with hot flushes;
- Regular exercise. “[I’ve] discovered yoga which has helped me anxiety-wise with mindfulness in particular,” says Jane.
- Taking Vitamin D, an over-the-counter supplement which helps the body absorb calcium and thus contributes to strong, healthy bones.
Then there’s hormone replacement therapy (HRT), which the NHS explains involves “using oestrogen to replace your body’s own levels around the time of the menopause”.
“I started taking HRT about 10 years ago before my periods stopped fully and felt amazing,” says Karen. “Due to high blood pressure and lumpy breasts, the gynaecologist has taken me off HRT”. That’s when Karen’s aforementioned menopause symptoms kicked in. Her symptoms now involve “loads of challenges which [...] make me feel generally rubbish and anxious which is not helpful when, as a solo entrepreneur, I need to be on top of my game!”.
Jane is currently on HRT. “As [I’m] still in the perimenopausal stage I take Utrogestan capsules for 14 days on, 14 days off but the Estradiol gel is applied daily,” she says.
Needless to say, though, HRT may not be right for everyone. Other treatments could include the following, as recommended by the NHS:
- Testosterone gel, if you’re looking to increase your libido;
- Cognitive behavioural therapy (CBT) if you’re struggling with low mood or anxiety, or if you want to talk through some of the physical changes happening in your body;
- Oestrogen for vaginal dryness, which can be inserted into the vagina (in the form of a cream, tablet or ring) – “I have an oestrogen cream that keeps the vagina supple,” says Karen.
Ultimately, though, ways to treat menopause symptoms will be different for everyone; and you should always speak with a healthcare professional if you’re worried or concerned.

Is there a link between probiotics and menopause symptoms?
Hanna warns that evidence is still emerging on the link between menopause and probiotics, that there is limited data on specific strains and ways of taking probiotics, and that studies are ongoing.
“However, the evidence for the use of probiotics to support vaginal health is promising,” she says. “Pre/probiotics can help with maintaining a balance of the microflora in the vagina, thus decreasing the chance of vaginal infections. Pre/probiotics – oral or vaginal – may also help decrease symptoms of vulvovaginal atrophy due to a lack of oestrogen caused by menopause.” This study would seem to agree: it noted that “probiotics combined with estrogen can alleviate the related symptoms caused by vulvovaginal atrophy”.
This Inspired Health article pointed to studies that found probiotics (most of which were various strains of Lactobacillus) could help with other menopause symptoms too (but added: “The direct relationship between probiotics and the relief of menopause symptoms is still a matter of ongoing research”). This is due to the highly beneficial impact of probiotics, especially Lactobacilli, on the gut microbiome. Menopause symptoms found to be improved by probiotics included:
- Osteoporosis
- Low mood
- Hot flushes
When it comes to treating menopause symptoms, nothing is guaranteed. But if you’re liking the sound of probiotics and want to give them a go, Daye’s ProViotics could be a good start.
Why, you ask? Well, they:
- Contain only live lactobacilli;
- Reach both the gut and the vagina alive;
- Are totally free from additives;
- Promote a diverse vaginal microbiota;
- Come with an expert seal of approval from Simon Gaisford FRSC CChem SRPharmS, Professor of Pharmaceutics at UCL School of Pharmacy.
Overall, though, as Hanna says: everyone’s body is different, especially when it comes to menopause. What works for one person (and, indeed, that person’s vagina) won’t necessarily work for someone else. So if something’s worrying you (or feels out of the ordinary at all), you should always speak to a healthcare professional first and foremost.
“[I] always was a bit sceptical about the menopause and how much it really affects women but my goodness I certainly don’t feel like that any more. It’s a tough gig!” says Jane – and we couldn’t agree more.







