Illustrated by Erin Rommel
If you have a cervix and are sexually active, you’ve likely heard of the human papillomavirus—or HPV, as it’s most commonly known.
Chances are, you’ve also had a smear test (or at the very least been invited to get one). For a virus that affects 80% of sexually active people, very few of us have a clear grasp on what the virus is and how it affects us. You can blame sexual stigma and fear mongering for that…
In occasion of International HPV Awareness Day (March 4th), here’s everything you need to know about HPV, what the virus entails, how it’s linked to cervical cancer, and whether you should be worrying about it.
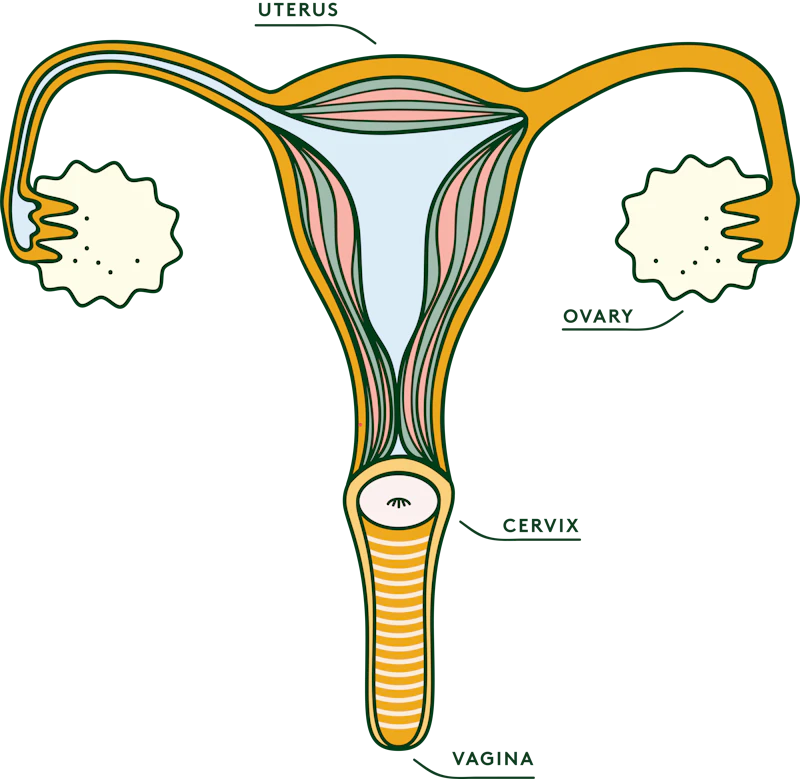
What is HPV?
Human papillomavirus (HPV) is a really common group of viruses. There are over 200 different types of HPV and most don’t cause any harm, but some types can cause certain cancers—these are known as “high-risk” HPV.
Is HPV an STI?
Although HPV is transmitted sexually, and certain strains of HPV can cause genital warts (a type of STI), HPV itself isn’t considered an STI.
How do you get it?
HPV is found everywhere in your body, including on your skin, but it’s usually passed on through sexual contact—whether it’s penetrative sex, oral sex, sharing sex toys or other forms of genital skin-to-skin contact.
Is HPV dangerous?
Sometimes, but in most cases, no. Most forms of HPV are harmless, but some forms of high-risk HPV can lead to the development of cancers like cervical, anal, genital cancer and cancer of the head and neck. 98% of cervical cancers are caused by HPV, specifically, types HPV16 and 18.
Some low risk types of HPV can also cause genital warts or verrucas, but these aren’t the same types of HPV linked to cervical cancer, so your risk of developing cervical cancer doesn’t increase even if you develop genital warts.
Can you prevent HPV?
It’s not entirely preventable, but there are a few ways o f protecting yourself from contracting HPV.
- Practice safe sex. Using a condom during penetrative sex can reduce your chances of contracting the virus.
- Get vaccinated. The free HPV vaccine is available in the UK for boys and girls aged 12 and 13. If you didn’t get the vaccine when you were younger, you can get it until the age of 25. You can also pay to get the HPV vaccine if you’re older than 25, but research shows it’s more effective if you have it at a young age.
- Get regular cervical screenings to detect HPV. In the UK, people with a cervix over the age of 25 are invited to routine smear tests (every 3-5 years).
Is the HPV vaccine effective?
In the UK, the national NHS HPV vaccine is called Gardasil. It protects against 4 types of HPV: HPV6 and 11 (which cause 90% of genital warts and are considered low-risk), and HPV16 and 18 (which are responsible for most cervical cancers and are considered high-risk).
The HPV vaccine is very safe and effective, and lasts for at least 10 years. New research also shows that a single dose of the vaccine is effective in preventing cervical cancer.
However, the Gardasil vaccine doesn’t protect you from all the types of HPV that cause cervical cancer, so it’s important to get routine smear tests!
How do I know if I have HPV?
You can’t know for sure! It’s incredibly common, and at least 8 out of 10 sexually active people have HPV—but they probably don’t know it. HPV doesn’t usually cause any visible symptoms, and it can lay dormant in your body for years.
Sometimes HPV will become active and cause problems, like genital warts, or cause cervical cells to change. So if your partner develops genital warts, it doesn’t immediately mean they’ve been cheating on you. Similarly, it’s why it’s so important to get regular cervical screenings even if you’ve been with your partner a long time, or haven’t had any sexual partners in a while.
Can HPV be treated?
Your immune system usually gets rid of HPV—sometimes within a matter of days, other times it takes a few years. Around 90% of HPV infections go away on their own within 2 years!
Annoyingly, the high-risk types of HPV can’t be cleared by your immune system and there isn’t a treatment. However, you can be given treatment for the complications it causes, like changes in cervical cells or genital warts.
What’s the link between HPV and cervical cancer?
Some forms of HPV can cause cervical cancer (note: this doesn’t mean that they will). Around 13 types of high-risk HPV are linked to cancer, with types 16 and 18 causing over 70% of cervical cancers.
For 1 in 10 people with a cervix, their immune system isn’t able to get rid of HPV (known as a persistent infection). We don’t really know why some people can’t fight off HPV, but in these cases, the HPV infection attacks cervical cells and causes them to change.
These “abnormal” cells are what doctors look for during a smear test if you have HPV, as over time they can turn into cancer. Regular cervical screenings are the best way to detect cell changes early, so they can be monitored or treated before they turn into cancer.
TL;DR
- Human papillomavirus (HPV) is a very common group of viruses. It's not an STI but it's passed on through sexual contact, and almost 80% of sexually active people have HPV.
- Your immune system usually gets rid of HPV on its own, but some types of HPV can cause verrucas and genital warts, while high-risk types of HPV can lead to cancer. Almost all cervical cancers are caused by HPV.
- HPV is not treatable, but it's highly preventable with a combination of vaccination and regular cervical screenings.