Table of contents
1. What are period cramps?
2. What causes period cramps?
3. How much period pain is ‘normal’?
4. How common are period cramps?
5. How can I treat, prevent or stop my period pain?
Illustrated by Erin Rommel, Sabrina Bezerra & Ralitza Nikolova
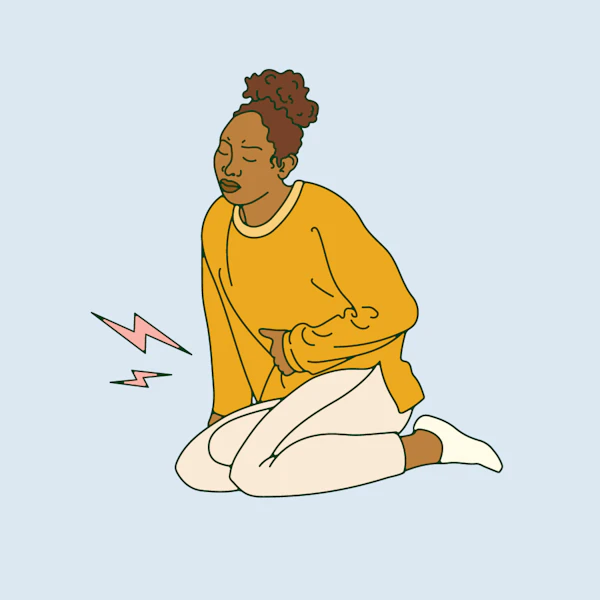
What are period cramps?
I’ll always remember a moment when I was reading Purple Hibiscus by Chimamanda Ngozi Adichie, a few years ago. At one point, the novel’s protagonist, Kambili, has period cramps. “Cramps racked my belly,” Kambili tells us. “I imagined someone with buckteeth rhythmically biting deep into my stomach walls and letting go.” And I thought: that’s it. That’s the best description I’ve ever read for the period pain I experience almost every month.
I’ve always found the singular, excruciating pain of period cramps hard to describe – hence why Adichie’s description struck such a chord with me. Sometimes, it’s like a steady burn: like someone’s slowly, steadily, repeatedly ripping a plaster away from my uterus. Sometimes it’s sheer agony: like my lower abdomen is being slowly, steadily, repeatedly sliced open.
Essentially, period cramps describe the pain experienced by uterus-owners during their period. “Period cramps can start in the days running up to your period and during it; usually easing as your period comes to an end,” says Dr Samantha Wild, GP and Clinical Lead for Women’s Health at Bupa Health Clinics. “The pain tends to affect your lower abdomen, and in some it also spreads to their lower back and thighs.” (I get pain around my upper thighs when the cramps are particularly bad.)
Painful periods can manifest differently for everyone. As Yoppie pointed out, there are many types of period pain. Some may experience an ongoing dull ache; others might suffer from a sharp poking sensation; others could notice an unpleasantly intense spasm.
And the period pain symptoms don’t stop there. “Along with cramps, some may get other symptoms before or during their period, including fatigue, diarrhea, nausea or sickness, headaches, bloating and feeling light-headed or more emotional than usual,” Wild continues.

What causes period cramps?
“Around the time of your period, your womb has more prostaglandins in it,” explains Wild. “Prostaglandins are chemicals that cause your womb’s muscles to tighten and help shed your womb’s lining. As these muscles tighten, the amount of blood and oxygen in your womb temporarily reduces, which triggers pain – this is known as primary dysmenorrhea.”
In other words, primary dysmenorrhea is all about uterine contractions – a phrase you may have heard before in conjunction with period pain – which help the uterus shed its lining each month.
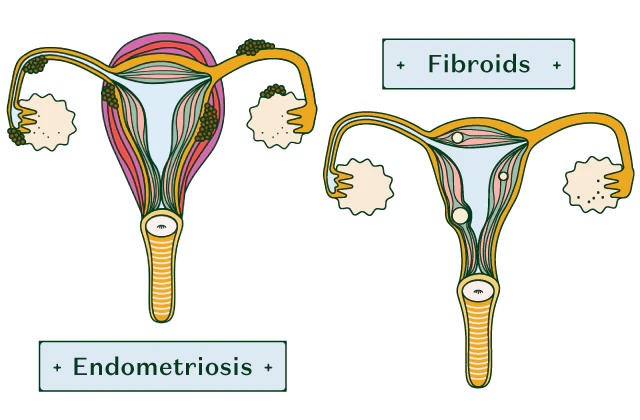
But period cramps aren’t necessarily always down to prostaglandins. “Some also get period cramps caused by an underlying medical condition like endometriosis or fibroids – this is known as secondary dysmenorrhea,” explains Wild. “Those with an underlying health condition experience more painful periods, as well as period pains at other times in their cycle, and worsening pain as their period progresses. It tends to affect those aged 30 to 45 more commonly.” Another possible cause of severe period pain could be PCOS: polycystic ovary syndrome.
More on secondary dysmenorrhea later. In the meantime, a third possible cause of period pain is posited by Wild: “Period cramps can also be caused by contraceptive devices like the coil, particularly in the first few months after it’s fitted,” she says.
How much period pain is ‘normal’?
“Period cramps can be unpleasant and inconvenient but in most cases, they don’t affect your ability to go about your day-to-day tasks,” says Wild. “[But] if you’re in severe pain that prevents you from doing what you would usually, or notice any changes to your usual period habits – like them becoming more irregular, longer or heavier – speak to a health professional for more guidance and possible treatment options.
“
56 percent of women felt the pain they experienced was ignored or dismissed.
How common are period cramps?
Sadly, they’re way too common. “Most people who have periods experience primary dysmenorrhea at some point in their lives,” says Wild.
She’s right. Around 90% of people with periods suffer with cramps; and yet the gender pain gap persists. To quote the BBC: “The gender pain gap is a form of discrimination within healthcare where unconscious medical bias contributes to women’s pain being written off either as a normal part of womanhood or as a matter of little relevance.”
Sounds bad? That’s because it is. Last year, the Independent drew attention to research commissioned by Nurofen and conducted via OnePoll, which surveyed 5,100 adults and found that “56 percent of women felt the pain they experienced was ignored or dismissed” and that period pain and endometriosis were significant pain culprits. “32 percent of women suffered from period pain as part of their daily lives, and 18 percent who experienced endometriosis pain experienced it for between three and five years,” the article explained.
So yes, period cramps are common: all the more so because women’s pain is so often dismissed or normalised, both in the healthcare sector and in society. The gender pain gap also points to a lack of knowledge and understanding around women’s pain, thanks predominantly to a lack of research.
“Currently, we don’t know why some people get period cramps more than others, but it’s thought that some retain more prostaglandins in the womb, so that may make their cramps feel stronger,” posits Wild.

How can I treat, prevent or stop my period pain?
- Immediate ways to reduce period pain:
Well, there’s the option of the aforementioned NSAIDs, or other over-the-counter painkillers, like paracetamol. Wild also puts forward the option of “transcutaneous electrical nerve-stimulation (TENS) machines – available from pharmacies – [which] send small electrical signals to the areas in pain.
“If you struggle with severe period pains, a health professional will offer treatments depending on whether you have primary or secondary dysmenorrhea,” Wild continues. “Hormonal contraception, prescribed painkillers and, in the worst cases, surgery can all be offered as possible treatments to reduce the impact of period pains.”
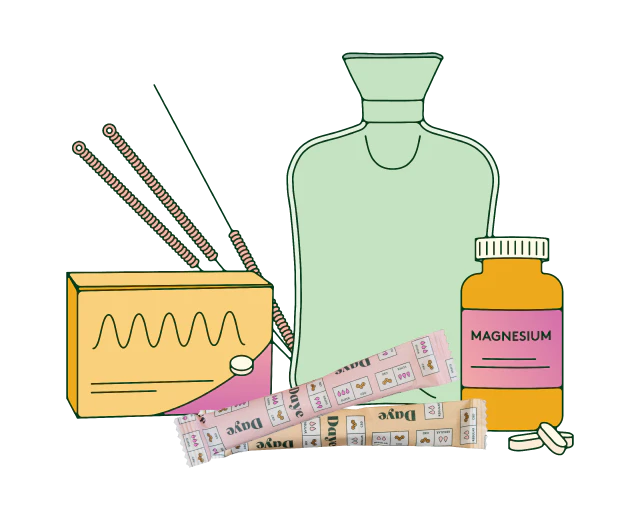
- Lifestyle changes to reduce period pain:
These lifestyle changes could also be known as natural or at-home remedies. “Heat can help soothe pain and help you relax – try a covered hot water bottle or heat patch applied to the tummy or back, or having a warm bath or shower,” says Wild. (Hot water bottles often help me, when it comes to soothing cramps.)
Other at-home remedies suggested by Wild include wearing loose-fitting clothing in the run-up to and during your period and gently massaging the painful areas. And other natural remedies still include:
- Magnesium supplements, which help relax the muscle of the uterus;
- Orgasms: the surge in both oxytocin and endorphins can do wonders for period pain;
- Pelvic floor stretches, such as yoga poses like cat/cow or child’s pose;
- Herbal tea, such as peppermint, chamomile or ginger;
Changing up your diet. For example, salmon is packed with omega-3s, which can help with reducing inflammation. Oats are rife with magnesium, which we already know relaxes the uterine smooth muscle and is also great for serotonin regulation; and bananas contain vitamin B6 and potassium (ideal for period cramp relief).
- Longer term lifestyle changes to reduce pain:
Wild suggests making certain types of exercise a regular part of your lifestyle routine – she cites the aforementioned yoga as an example – and says, “If you’re a smoker, stopping may ease period pains”.
Ultimately – although the gender pain gap persists – it’s always worth making an appointment with a healthcare professional if you’re in any way concerned, or if you simply need some period pain relief. As Wild says: “If you’re concerned about the heaviness, regularity or length of your periods, have blood clots that are around the size of a 10p coin or experience debilitating symptoms around your period, you should always make the time to see a health professional to discuss your symptoms and see whether [there are] any ways to reduce what you go through each month”. Amen to that.