Table of contents
1. If you’ve ever woken up in the morning to find that your maxi pad wasn’t enough to tame your flow, or you’ve had to rush to the bathroom because of an overflowing Super Plus tampon, you can probably relate to the struggle of having a heavy period.
2. Why is my flow so heavy?
3. What blood clots during your period mean
4. Can a heavy period cause anaemia?
5. How to manage heavy periods
6. Can tampons make periods lighter?
Illustrated by Sabrina Bezerra
If you’ve ever woken up in the morning to find that your maxi pad wasn’t enough to tame your flow, or you’ve had to rush to the bathroom because of an overflowing Super Plus tampon, you can probably relate to the struggle of having a heavy period.
Rest assured that you’re not alone. It’s estimated that one in three women in the UK have a heavy period, with one in 20 consulting their GP every year for this same reason.
A heavy period (menorrhagia) may be a nuisance but most of the time they’re not something to worry about. In some cases, however, heavy periods can cause disruption to your day-to-day, emotional distress, and in rare cases lead to anaemia.
From contraception side effects to more serious reproductive health conditions, keep reading for some common reasons why you might be experiencing a heavy flow, and tips on how to manage heavy periods.
What is a ‘normal’ flow?
Not all periods are created equal, so there’s no such thing as a ‘normal’ period.
As with most things related to reproductive health, it’s not one-size-fits-all – that’s why some of us reach for the Super tampons, and others can get away with nothing but a panty liner.
The amount of blood you lose on your period varies from woman to woman, but on average you lose around 6-8 teaspoons (30-40ml).
How heavy is too heavy?

What constitutes heavy flow is very subjective. A ‘heavy’ period used to be characterised as one where you lose 80ml or more of blood each period, have periods that last longer than a week, or both.
Modern guidelines now classify heavy periods as any amount of menstrual bleeding that impacts your quality of life – which is objectively an easier definition than having to measure the volume of your menses!
Other key features of a heavy period are:
- Having to change your pad or tampon every hour
- Passing blood clots larger than 2.5cm
- Routinely bleeding through your clothes or onto your bed sheets
- Having to use two types of period product together – like a tampon and pad at the same time
- A period looks like *that* scene from The Shining…
The NHS website has a handy self-assessment tool to help you figure out if you have heavy periods.
Usually, a heavy flow is not cause for concern, but if you notice that your bleeding pattern changes unexpectedly, or you have unusual vaginal bleeding (like in between periods or after intercourse) then you should let your GP know.
Why is my flow so heavy?
There is no single cause for a heavy period. Anything from your stress levels, diet, general lifestyle, contraception and other medications can all affect your period.
Sometimes a heavy period isn’t caused by anything in particular, but in other cases it can be due to a serious underlying issue.
Fibroids
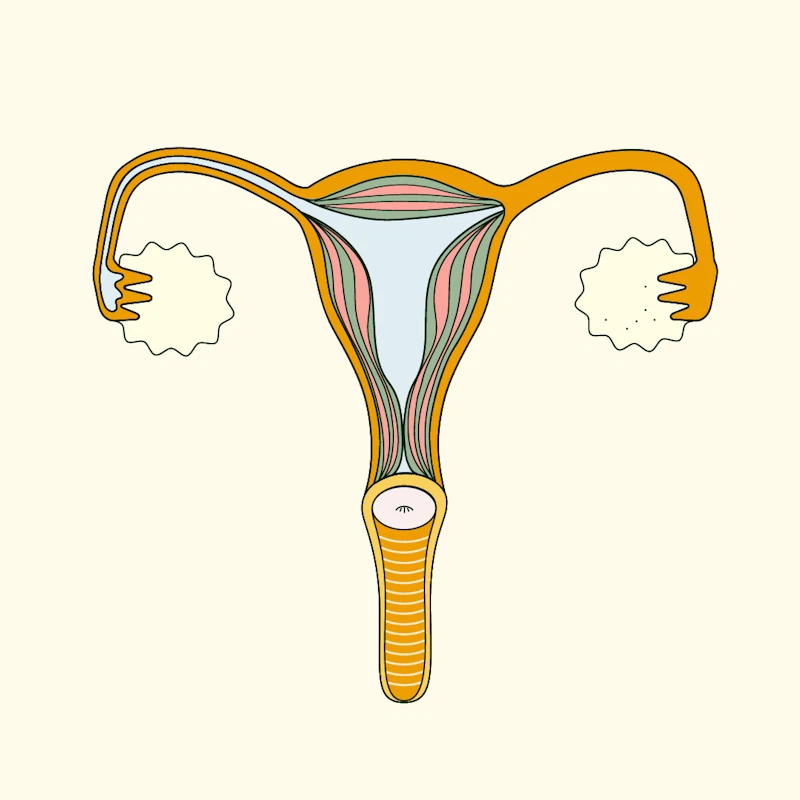
Uterine fibroids are benign (non-cancerous) growths found in, on and around the uterus. They’re a common cause of heavy periods, pelvic pain and bleeding between periods.
Fibroids are pretty common, and most women will experience uterine fibroids at some point in their lives. Most fibroids are small and cause no symptoms, to the point where you may have fibroids and not even know.
Fibroids also typically shrink on their own once you reach menopause.
20-50% of women of reproductive age have fibroids, but you’re more likely to get them when you’re older.
Endometriosis
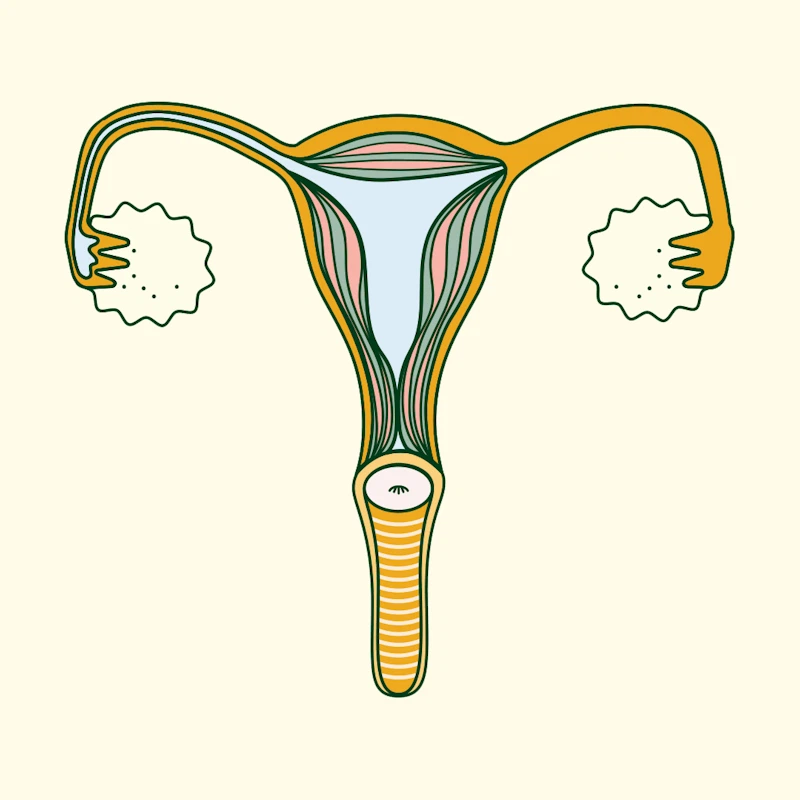
Endometriosis is a condition where cells similar to the uterine lining start to grow in other places of the body, including the ovaries, fallopian tubes, and bowels. It can cause severe pain and, often, irregular and heavy periods.
Endometriosis is not technically a cause of heavy bleeding, but the two often go hand in hand.
The copper coil
Copper IUDs are commonly associated with heavy bleeding. Painful, heavier periods are a common, temporary side-effect of IUDs. Your flow should go back to normal after a few months of inserting the IUD.
However, many women report having a heavier flow with an IUD as a permanent side effect. Although this is just anecdotal evidence, if you already experience heavy periods it may be worth considering an alternative method of contraception.
The hormonal IUS, for example, has the opposite effect of an IUD, and can actually make your periods lighter – or stop altogether.
Stress
Stress can have a huge impact on your overall health, including your periods.
When you’re stressed, your brain signals your body to produce two hormones: corticotropin-releasing hormone (CRH) and cortisol, aptly dubbed the “stress hormone”.
Increased CRH and cortisol can suppress normal levels of oestrogen and progesterone, the hormones that control your menstrual cycle.
There’s no one way your period may be affected when you’re stressed, but too much stress can cause your period to become heavier, more painful, irregular or even cause it to go MIA.
Bleeding disorders
In rare cases, a heavy flow could be caused by a bleeding disorder.
Your body produces blood clotting agents called coagulants as a way to stop bleeding and limit the amount of blood loss – including when you’re on your period.
If you have a coagulant deficiency, or a blood clotting disorder like Von Willebrand’s Disease, this can cause your periods to be longer and heavier.
What blood clots during your period mean
Blood clots are a common feature of periods, and typically nothing to worry about. Clots are made up of coagulated blood and endometrial tissue, and they can look like chunks and/or a jelly-like consistency that can vary in size.
During your period, hormonal fluctuations trigger your body to shed your uterine lining, which exposes blood vessels in your uterus and causes them to bleed.
In order to speed things along, your body produces anticoagulants to break down the blood and tissue so it can pass through your cervix more easily.
When you have a very heavy flow, sometimes your body doesn’t produce enough anticoagulants in time, causing clots.
This could also explain why you’re more likely to experience more intense cramping if you have a heavy flow – your uterus needs to work overtime and contract even more in order to pass large blood clots.
When to see a doctor about period blood clots
Noticing blood clots on your pad or tampon is a normal part of having a period, especially on your heaviest day or if you have a heavy flow.
Period blood clots aren't always a cause for alarm, but there are caveats. If you notice persistent blood clots that are larger than 2.5cm, if you experience severe fatigue and dizziness while on your period, or if the heaviness of your flow concerns you, you should speak to your GP.
Can a heavy period cause anaemia?
Heavy periods can sometimes cause anaemia, a blood disorder where you have lower levels or red blood cells and haemoglobin (a protein present in red blood cells responsible for carrying oxygen from the lungs to cells in the body).
Common symptoms of anaemia include:
- Paleness
- Fatigue
- Headaches
- Shortness of breath
- Dizziness
Anaemia has several possible causes, one of which is heavy periods. When you have a heavy flow, you can end up losing more red blood cells than your body can make. This lowers the levels of iron, an essential nutrient needed for your body to produce haemoglobin.
If you’re anaemic as a result of heavy periods, your doctor may recommend taking iron supplements or eating more iron-rich foods.
How to manage heavy periods
If your period is so heavy that it’s interfering with your quality of life, you have every right to seek a solution!
There’s no specific treatment for heavy periods, but there are different options available to help lessen menstrual bleeding and manage symptoms.
Medications
The first-line treatment for menorrhagia is usually hormonal contraception like the IUS, which releases low levels of synthetic progesterone and keeps the uterine lining thin, reducing menstrual flow. It can take up to six months before you notice lighter periods with an IUS.
Similarly, the combined oral contraceptive pill can also be used to manage heavy or painful periods. It works by preventing ovulation and keeping the uterine lining thin, stopping periods completely.
The menstrual bleeding you may experience on the pill isn’t a real period, but rather a withdrawal bleed. If you’d rather not bleed at all, you can take the pill back to back and skip the pill-free week.
If an IUS or the pill aren't a suitable option, you may be prescribed tranexamic acid, a medication that helps the blood in your uterus to clot. Tranexamic acid tablets are taken when your period starts, for a maximum of four days.
Non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen, mefenamic acid and naproxen can also reduce menstrual bleeding. They work by inhibiting your body’s production of prostaglandins, hormone-like chemicals that cause your uterine muscles to contract and help shed your endometrium. Prostaglandins are what cause period cramps and have been linked to heavy periods.
Mefenamic acid and naproxen are only available via prescription, and you shouldn’t take ibuprofen to stop or delay your period without the supervision of your doctor.
Surgical procedures & non-surgical interventions
There are several procedures and surgical interventions that can treat heavy menstrual bleeding. These include:
- Endometrial ablation, which involves thinning, removing or destroying the endometrium by cutting off the blood supply. Menstrual bleeding doesn’t always stop in these cases.
- Uterine artery embolisation (UAE), a non-surgical procedure used to shrink fibroids. This is an option commonly used for women who want to treat menorrhagia while preserving their fertility.
- Hysterectomy, an invasive and complicated surgery to remove the uterus.
Can tampons make periods lighter?
The simple answer to that is: nope. Despite what you may have read on the internet, no period product can change how heavy your flow is.
That being said, finding the right period product for your body and flow can help you manage it.
If you have a heavy flow, it’s important that you’re using period care designed for it. It may not make your flow lighter, but it will give you much more peace of mind.







